Increased sedentary time from childhood through young adulthood worsened low-grade inflammation in a new study. However, the results also showed that light physical activity (LPA) may completely reverse the adverse process. Moderate-to-vigorous physical activity (MVPA) did not have a similar effect. The study was conducted in collaboration between the University of Bristol in the U.K., the University of Exeter in the U.K., and the University of Eastern Finland, and the results were published in The Journal of Clinical Endocrinology & Metabolism.
Low-grade inflammation has been associated with several diseases throughout the lifespan, ranging from cardiovascular, metabolic, neurological, and musculoskeletal diseases to cancer. Moreover, it was recently established that low-grade inflammation may contribute to premature vascular damage in adolescents and young adults.
More than 80% of adolescents across the globe have insufficient physical activity per day as reported by the World Health Organization. It is estimated that physical inactivity will have caused 500 million cases of heart disease, obesity, diabetes, or other noncommunicable diseases by 2030, which is estimated to cost US$ 27 billion annually.
This alarming forecast regarding the morbid danger of physical inactivity necessitates urgent research on the most effective preventive approach.
The long-term role of movement behavior, objectively measured with an accelerometer, in low-grade inflammation in the pediatric population has not been previously studied. This is due to the cost and other challenges of repeatedly measuring movement behavior in the same cohort during growth from childhood through young adulthood, with such studies lasting more than 10 years.
The current study which used data from the University of Bristol study Children of the 90s (also known as the Avon Longitudinal Study of Parents and Children) included 792 children aged 11 years who were followed up until age 24 years, with a total follow-up time of approximately 13 years. Accelerometer measures of sedentary time, LPA, and MVPA were collected at ages 11, 15, and 24 years. High sensitivity C-reactive protein, a marker of inflammation, was repeatedly measured at ages 15, 17, and 24 years.
These children also had dual-energy X-ray absorptiometry measurements for total body fat mass and skeletal muscle mass, as well as fasting blood samples such as glucose, insulin, high-density lipoprotein cholesterol, low-density lipoprotein cholesterol, triglyceride, smoking status, socio-economic status, and family history of cardiovascular disease repeatedly measured at ages 15, 17, and 24 years.
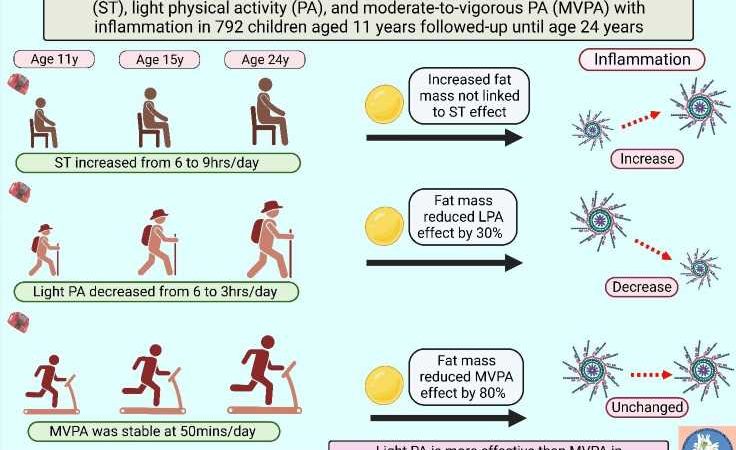
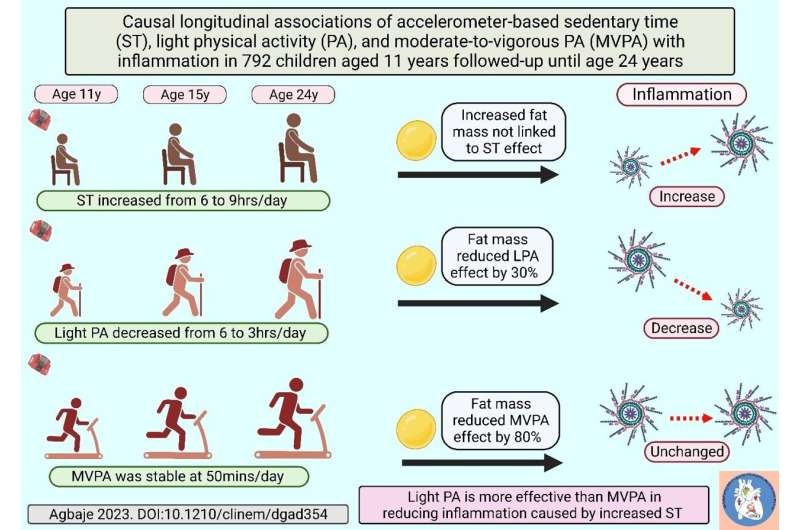
During the 13-year follow-up, sedentary time increased from approximately six hours/day in childhood to nine hours/day in young adulthood. LPA decreased from eight hours/day to three hours/day while MVPA was relatively stable around 50 mins/day from childhood until young adulthood. It was observed that increased sedentary time significantly worsened inflammation, partially by raising blood pressure. Increased blood pressure explains only 8% of the relationship between sedentary time and inflammation.
LPA from childhood through young adulthood was associated with reduced inflammation, however, increasing body fat mass reduced the effect of light physical activity by 30%. MVPA from childhood was associated with reduced inflammation but increased total fat mass decreased the effect of MVPA by 80%. The significant impact of fat mass effectively neutralized the effect of MVPA on inflammation.
“We are seeing for the first time that LPA from childhood may be better than MVPA at reversing the adverse effect of sedentary time on worsening inflammation. It is rather surprising that the physiologic increase in total fat mass even in healthy-weight children remarkably blunted the effect of MVPA on lowering inflammation,” says Andrew Agbaje, a physician and clinical epidemiologist at the University of Eastern Finland.
“We have also recently reported that LPA promotes healthy hearts among adolescents better than MVPA. These findings emphasize that LPA may be an unsung hero in preventing diseases from early life, and in this regard it could be 2–3 times more effective than MVPA,”
“The World Health Organization has only emphasized that children and adolescents should accumulate on average 60 mins of MVPA per day and reduce sedentary time. There has been almost no guideline on engaging in LPA in the young population because data is lacking. Our recent studies are now contributing to this body of evidence. Therefore, public health experts, pediatricians, and health policymakers should encourage more participation in LPA from childhood. However, more research on the health benefits of LPA is needed to provide sufficient evidence for updating current health guidelines,” Agbaje continues.
More information:
Andrew O Agbaje, Longitudinal Mediating effect of Fatmass and Lipids on Sedentary Time, Light PA, and MVPA with Inflammation in Youth, The Journal of Clinical Endocrinology & Metabolism (2023). DOI: 10.1210/clinem/dgad354
Journal information:
Journal of Clinical Endocrinology & Metabolism
Source: Read Full Article