Moyamoya is a rare blood vessel condition that has an outsized impact on children, as it is responsible for about 6 percent of pediatric strokes in the United States. Surgical revascularization is the only treatment and is very effective. However, clinicians face challenges in identifying new or worsening disease before a disabling stroke occurs, predicting optimal timing for surgical intervention, and tailoring treatment to individual patients. These challenges are further exacerbated in children, who may not be able to articulate symptoms clearly or tolerate the detailed imaging tests commonly used in adult patients.
Now, results from a recent proof-of-concept study by Edward Smith, MD, Darren Orbach, MD, Ph.D., and their colleagues in the Cerebrovascular Surgery and Interventions Center at Boston Children’s Hospital reveal a promising new noninvasive biomarker test for moyamoya. This groundbreaking work, built on the foundation of tumor-related biomarkers developed in Smith’s lab at the Vascular Biology Program, highlights Boston Children’s unique ability to bring together clinicians and scientists in pursuit of innovation.
First-of-its-kind finding for moyamoya
Led by Julie Sesen, Ph.D., in the Vascular Biology Program, the team analyzed urine and cerebral spinal fluid (CSF) specimens collected from 32 pediatric moyamoya patients prior to surgery at Boston Children’s between 2009 and 2016. They also analyzed specimens from matched healthy patients who served as controls. The moyamoya patients had extensive medical records and detailed imaging studies, providing the scientific team an incredible wealth of clinical data to correlate with the biomarker development.
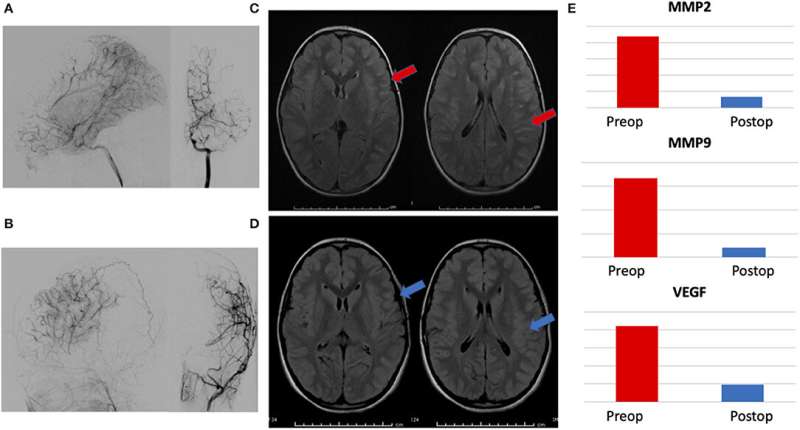
In evaluating the specimens for urinary and CSF biomarkers, the team found significant elevations of angiogenic proteins in samples from moyamoya patients, compared with control patients. These included the urinary biomarkers MMP-2, MMP-9, MMP-9/NGAL, and VEGF. Of these, MMP-2 was the most optimal biomarker, with a sensitivity of 88 percent, specificity of 100 percent, and overall accuracy of 91 percent. Levels of MMP-2 changed in response to treatment and also correlated with radiographic evidence of revascularization.
Laying the foundation for future care
Source: Read Full Article
